
The Map Has Blind Spots
Move 37 was not a parlor trick. It was a warning. Physician-developers need to be ready for the moment AI starts finding medically important patterns our inherited maps never taught us to see.

Move 37 was not a parlor trick. It was a warning. Physician-developers need to be ready for the moment AI starts finding medically important patterns our inherited maps never taught us to see.

HealthBench Professional shows AI has already crossed the threshold in clinical writing and documentation. The real lesson is not replacement. It is that physician-developers need to build the harness.

Joe Riley trusted AI over his oncologist and died of a treatable cancer. His tragedy wasn't naivety — it was earned distrust, amplified by a machine that had no way to know the difference.

An app on your laptop helps no one. Deployment is the step where physician-developer work finally becomes available to patients, colleagues, and clinics.

Clinical software becomes real when it remembers. This is the database layer that turns a one-off calculator into a longitudinal tool.
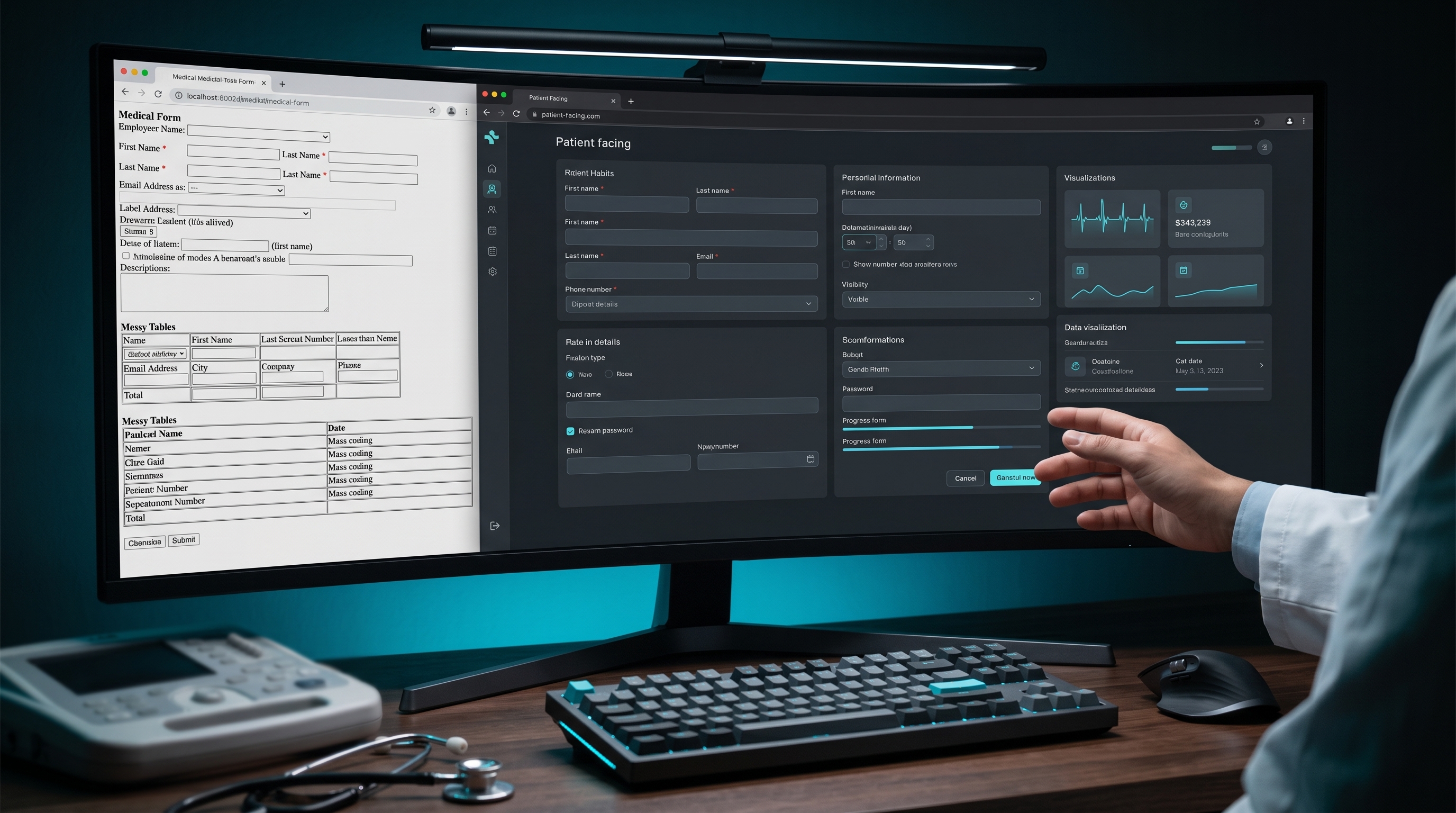
Patients do not trust ugly calculators. Tailwind helps physician-developers build interfaces that feel clean, credible, and ready to use.

Physician-developer projects are usually content-first. Astro fits that shape by shipping less JavaScript, faster pages, and cleaner performance by default.
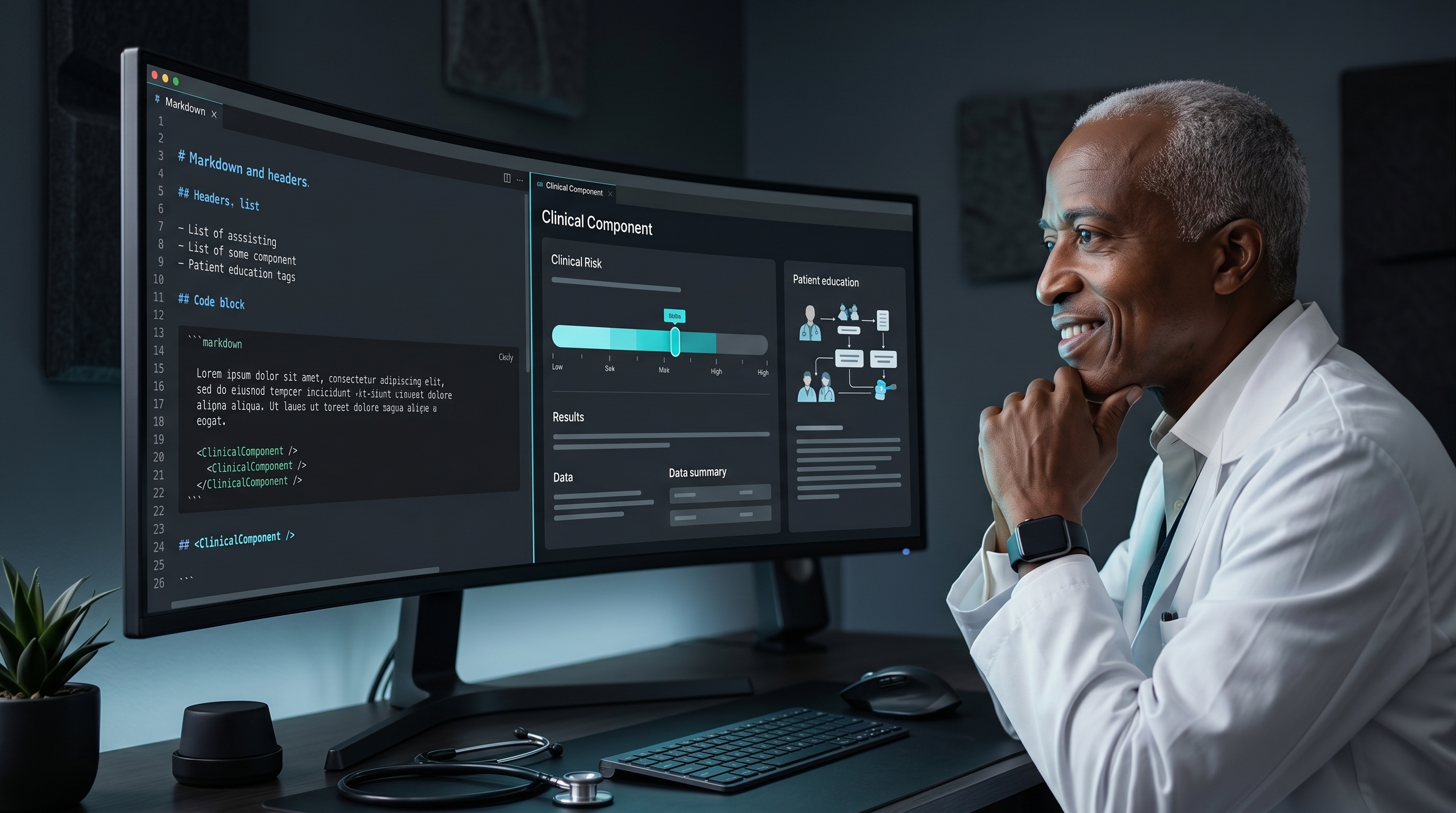
Most physician writing dies in static documents. MDX turns clinical education into living pages that can explain, calculate, and update in one file.

Claude Code, Cursor, and Copilot do not replace judgment. They compress the feedback loop for physician-developers who still read every line before they ship.

JavaScript runs in the browser. Python runs behind the workflow, where lab values, CSV exports, data cleaning, and clinical models actually live.

Clinical software cannot afford vague inputs. TypeScript gives physician-developers safer contracts, clearer data shapes, and fewer silent failures.
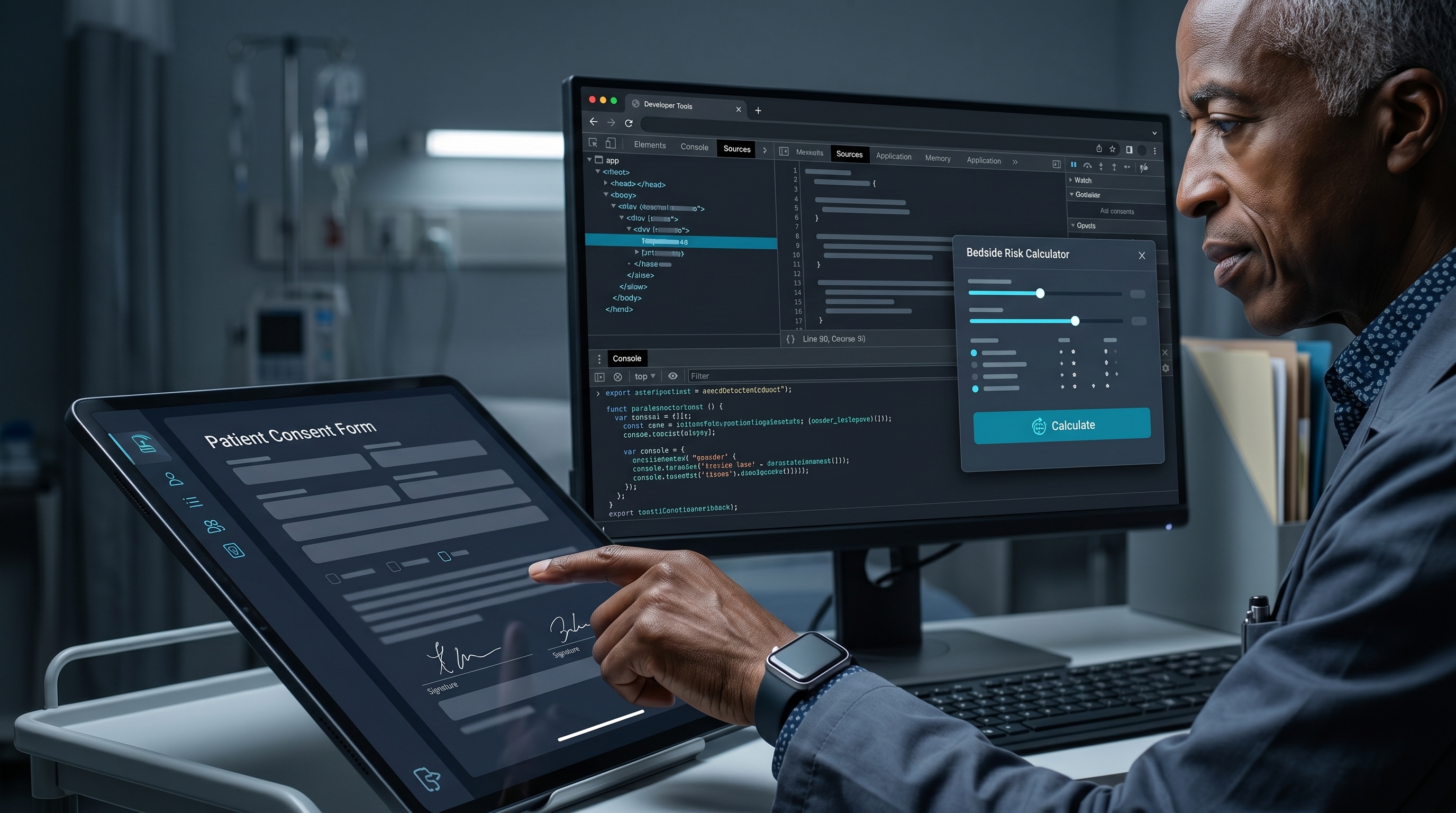
Every patient portal, tablet consent form, and browser-based clinical tool already runs JavaScript. This is where physician-developers start changing what medicine feels like on a screen.

A practical 10-part Doctors Who Code series for physicians who want to build and ship clinical tools with the modern web stack, from JavaScript to deployment.

Deep work is not a productivity hack for doctors. It is a clinical safety issue, a training issue, and a systems design issue. Physicians need to protect deep thinking and automate the shallows.

AI agents are 50x faster than humans, but medicine only captures a fraction of that speed. The real bottleneck in agentic AI is not the technology — it is human capacity, clinical oversight, and workflows built for the wrong consumer. A physician-developer's perspective.

Consumer AI tools like ChatGPT and Claude are useful. But a physician-developer who deploys a locally fine-tuned model on controlled infrastructure has something more powerful: a clinical tool that learns your practice, respects your data, and costs less at scale.

Documentation automation is not a typing solution. It is a workflow design problem. For physicians and physician-developers, the real goal is protecting clinical judgment from administrative drag.

PGIS Recipes started as a stack of Marp slide decks. I turned it into a GitHub Pages library because nutrition guidance only compounds when the delivery system is structured, durable, and easy to revisit.

Not to become programmers. To become the kind of physician who can close the gap between a clinical insight and a working solution.

A TEDx pitch says physicians should build AI. I agree. But the work that matters is governance, validation, and delivery, not one-afternoon demos.

Physicians do not have an information problem. We have a conversion problem. Inside the Telegram-driven research engine I built to turn links, papers, transcripts, and videos into drafts, PDFs, and durable editorial records.
A practical path for physicians who want to move from GitHub basics to building real medical AI projects.

Most physician-developers never ship their first AI project. The problem is not skill. It is scope. Here is a framework for choosing a project that lands.

There are thousands of medical AI repositories on GitHub. Most are abandoned, half-built, or unreproducible. Here is how to find the ones that actually work.
A physician's guide to JSON, FHIR JSON, and structured clinical data for APIs, interoperability, and medical AI.

Most physician-developer projects fail not because the ideas are bad but because the first build is too large. Here are three that are sized to finish.

Not a tutorial on becoming a developer. A seven-day plan for a busy physician to go from zero to a real project in a repository they will actually return to.

Most physician-developers lose code the same way: no backups, no history, no way to recover. Here is why version control matters.

Most physicians assume GitHub is for real developers. That assumption is costing medicine. Here is why the barrier is not skill, and what to do instead.

Nobody lost your fax. The system was designed to lose it. Referral failures are not clerical accidents. They are the predictable result of clinical infrastructure built for a different era.

Race-based clinical algorithms in kidney care and obstetrics did not just reflect bias. They operationalized it. Physicians now have a responsibility to challenge the software, logic, and architecture that turn racial fiction into patient harm.
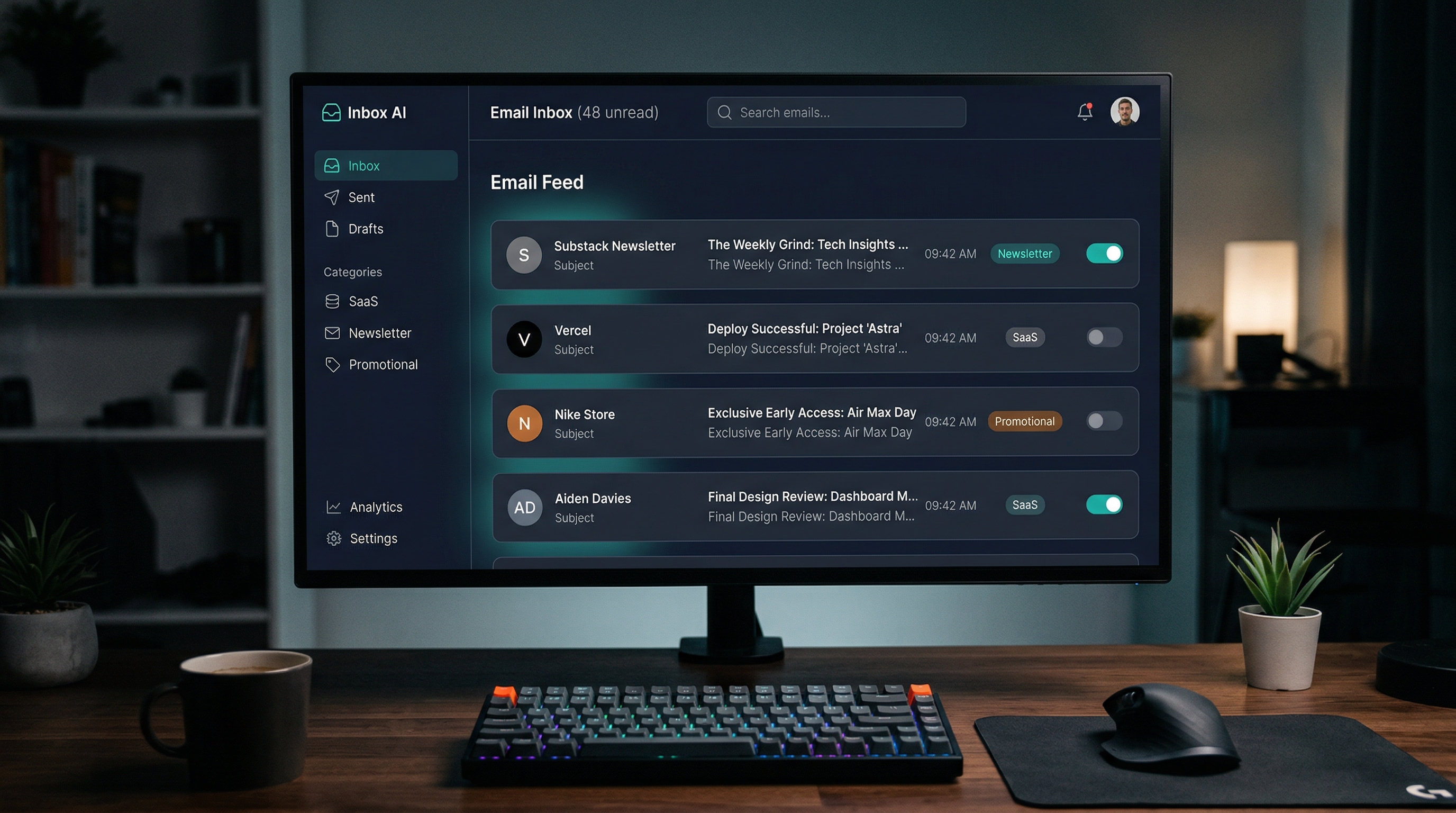
InboxDetox is an AI-powered email unsubscribe manager built in two evenings and deployed to Railway. It is on GitHub. Take it.

A practical breakdown of 2025 CPT telehealth codes, RPM billing thresholds, and the workflow engineering required to make digital medicine financially sustainable.

They are not asking it for fun. They are asking it because the triage line puts them on hold for 45 minutes. The threat is not the technology. The threat is the system that made the technology necessary.

Physician passivity in health tech is not an accident. It is a business model. Understanding the structural incentives is the first step to building outside of them.

Before you build any AI feature, you must first build the log. The principle every physician-developer needs to internalize before writing a single line of intelligence code.

Every physician who codes started somewhere that had nothing to do with clinical AI. The first build is about identity formation, not impact. Here is why that distinction matters, and where to actually start.

When families face periviability, they search before they call. What they find shapes everything. Here is why physician-developers have a responsibility to build better.

Every physician using an AI tool has heard the liability question. Most of us answer it wrong. The real answer is not about insurance. It is about who was in the room when the tool was designed.

The AMA opened the door. Physicians must decide what to do with it. The survey data is not a comfort. It's a challenge. Here's what physician-developers do next.

88% of physicians fear AI will erode their clinical instincts. That fear is real but misdirected. The greater risk is intellectual dependency on systems we didn't build and cannot interrogate.

The AMA's 2026 survey shows 81% of physicians now use AI in practice. But read the fine print. Physicians want a seat at the table. The best way to earn that seat is to be the person who wrote the code.

After spending a day fighting a WordPress plugin that wouldn't respect a domain change, I rebuilt DoctorsWhoCode.blog from scratch with Astro and MDX. The migration took one afternoon. The clarity was immediate.

A physician-developer explores the powerful parallels between AI-driven glycemic control in the ICU and metabolic management for endurance athletes with Type 2 diabetes, introducing the Performance Glycemic Intelligence System (PGIS) as a real-world n-of-1 framework.
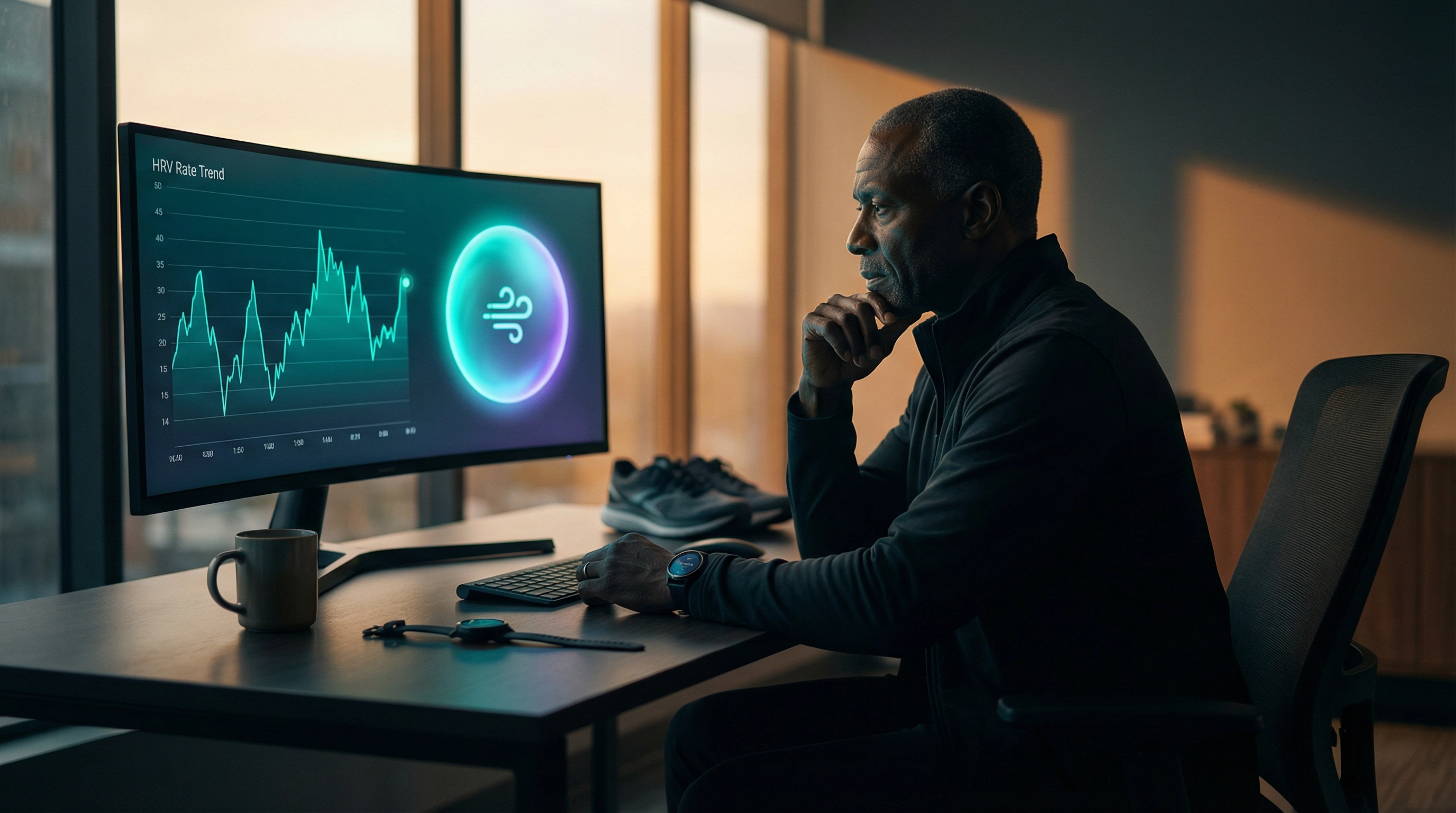
A Maternal-Fetal Medicine specialist describes how his personal AI health system identified low HRV, recommended breathing exercises, and prompted him to build a custom evidence-based breathing app in a single afternoon. A case study in disposable software, physician agency, and the future of personal health technology.

By Dr. Chukwuma Onyeije, MD, FACOG | Maternal-Fetal Medicine Specialist & Medical Director, Atlanta Perinatal Associates

It was a Tuesday evening consult. A doctor called with a patient at 31 weeks small for gestational age, elevated umbilical artery resistance, and a wo...
Maternal-Fetal Medicine Specialist, Medical Director at Atlanta Perinatal Associates, Founder of CodeCraftMD
Maternal-Fetal Medicine Specialist | Founder, CodeCraftMD | Atlanta Perinatal Associates
Maternal-Fetal Medicine Specialist & Founder, CodeCraftMD
Maternal-Fetal Medicine Specialist & Founder, CodeCraftMD

For the past two decades, medical software has been synonymous with monolithic platformsEpic, Cerner, and their ilkmassive systems designed to serve e...
I'm a maternalfetal medicine physician managing complex, high-risk pregnancies. I have long-standing type 2 diabetes. And right now, I'm training for m...
> Keywords: AI clinical documentation, ambient transcription, EvidenceMD, CodeCraftMD, physician automation, clinical workflow, medical billing automati...

A step-by-step tutorial for physician-developers on authenticating with the Epic FHIR sandbox, making your first API call in Python, and building toward a SMART on FHIR clinical app -- no enterprise contract required.